DIFFERENTIAL DIAGNOSIS OF CHEILITIS – HOW TO CLASSIFY CHEILITIS?
DIFFERENTIAL DIAGNOSIS OF CHEILITIS – HOW TO CLASSIFY CHEILITIS?
Acta Clin Croat. 2018 Jun; 57(2): 342–351.
doi: 10.20471/acc.2018.57.02.16
PMCID: PMC6531998
PMID: 30431729
Liborija Lugović-Mihić,1,2 Kristina Pilipović,2 Iva Crnarić,1 Mirna Šitum,1,2 and Tomislav Duvančić1
Author information Article notes Copyright and License information Disclaimer
Abstract
SUMMARY – Although cheilitis as a term describing lip inflammation has been identified and recognized for a long time, until now there have been no clear recommendations for its work-up and classification. The disease may appear as an isolated condition or as part of certain systemic diseases/conditions (such as anemia due to vitamin B12 or iron deficiency) or local infections (e.g., herpes and oral candidiasis). Cheilitis can also be a symptom of a contact reaction to an irritant or allergen, or may be provoked by sun exposure (actinic cheilitis) or drug intake, especially retinoids. Generally, the forms most commonly reported in the literature are angular, contact (allergic and irritant), actinic, glandular, granulomatous, exfoliative and plasma cell cheilitis. However, variable nomenclature is used and subtypes are grouped and named differently. According to our experience and clinical practice, we suggest classification based on primary differences in the duration and etiology of individual groups of cheilitis, as follows: 1) mainly reversible (simplex, angular/infective, contact/eczematous, exfoliative, drug-related); 2) mainly irreversible (actinic, granulomatous, glandular, plasma cell); and 3) cheilitis connected to dermatoses and systemic diseases (lupus, lichen planus, pemphigus/pemphigoid group, angioedema, xerostomia, etc.).
Key words: Cheilitis, Inflammation, Lip Diseases, Actinic Cheilitis, Classification, Dermatitis, Contact
Introduction
The term cheilitis indicates inflammation of the lip and includes many types, i.e. angular, contact, exfoliative, actinic, glandular, granulomatous, plasma cell cheilitis, simplex, etc. (1–5). In practice, it is difficult to define readily the precise type of cheilitis, thus proper diagnostic procedures are necessary to determine the exact disease based on its characteristics (5). For example, angular cheilitis can occur spontaneously or may be related to several precipitating factors (e.g., systemic immune suppression, local irritation and moisture, fungal/bacterial infection). Contact cheilitis can be related to the effects of irritants (climatic, mechanical, caustic agents) or allergens (allergic contact cheilitis) (5). Some types of cheilitis last longer and are persistent, such as chronic actinic cheilitis, granulomatous cheilitis and plasma cell cheilitis. Furthermore, cheilitis can also be seen in various skin or systemic diseases such as lupus erythematosus, lichen planus, atopic dermatitis, etc.
Cheilitis may also be associated with numerous conditions or diseases, e.g., nutritional deficiencies, such as megaloblastic anemia due to vitamin B12 deficiency, anemia due to iron deficiency, oral candidiasis, diabetes (2, 4–8).
Additionally, cheilitis is often divided into particular subtypes with no clear classification having yet been adopted. Considering its duration, some authors refer to acute or chronic cheilitis, whereby there are no clear criteria (2). Although there are many recent papers on cheilitis, they are mostly case reports and overviews of therapeutic or diagnostic procedures based on personal experiences and results without specific criteria for classification. Since clear classification has not yet been established, there are no definitive recommendations for diagnosing all different types of cheilitis. Apart from that, cheilitis is also a disease that requires a multidisciplinary approach, which additionally complicates adoption of a classification system. We would like to put forth a classification of cheilitis into three main groups with further particular subtypes (Table 1).
Table 1
Proposed classification of cheilitis
| Mostly reversible | Mostly persistent | In association with dermatoses and systemic diseases (common diseases) |
| Cheilitis simplex Angular/infective cheilitis Contact/eczematous cheilitis Exfoliative cheilitis Drug related cheilitis |
Actinic cheilitis Granulomatous cheilitis Glandular cheilitis Plasma cell cheilitis |
Lupus erythematosus Lichen planus Angioedema Pemphigoid/pemphigus Xerostomia Erythema multiforme Crohn’s disease Sarcoidosis, etc. |
Reversible Cheilitis
We specify reversible cheilitis (transitory cheilitis of temporary duration) as a distinct category, which includes several subtypes (Table 2).
Table 2
Prominent features of mostly reversible cheilitis
| Mostly reversible cheilitis | Occurrence | Related factors | Therapy |
| Cheilitis simplex | Common | Lip licking Cold, windy, dry weather |
Advice on environmental conditions Application of lip balms, petroleum jelly, emollients, topical corticosteroids, ointments |
| Angular/infective cheilitis | Common | Infective agents Immune deficiency (diabetes, HIV) Mechanical factors Nutritional deficiencies (riboflavin, folate, iron, etc) |
Elimination of local predisposing factors Topical antimycotics, antiseptics, antibiotics, topical corticosteroids |
| Contact/eczematous cheilitis | Very common | Atopy, contact allergens/irritants | Topical corticosteroids (low to medium potency), emollients |
| Exfoliative cheilitis | Rare | Lip licking/picking Psychological distress Nutritional deficiencies |
Corticosteroids Psychotherapy (some cases resolve spontaneously) |
| Drug related cheilitis | Rare | Drugs | Emollients Drug elimination if possible |
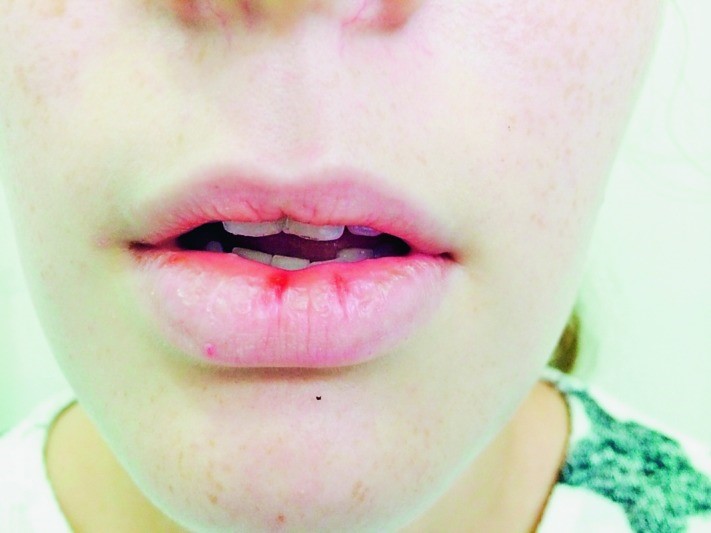
Cheilitis simplex (chapped lips, common cheilitis, cheilitis sicca) is one of the most common subtypes, presenting as cracked lips, fissures or desquamation of the lips, usually of the lower lip (Fig. 1) (2, 7). Here frequent lip licking promotes dryness and irritation, ending in separation of the mucosa and cracking. Some authors use a different label for a similarly categorized subtype, lip licking cheilitis, due to lip licking habit or frequent lip retraction into the oral cavity (especially in children with atopic dermatitis) (6, 7). Such licking removes the thin, oily surface film that protects the lips from moisture loss, leading to lip cracking. Lip lesions are also influenced by saliva, the digestive enzymes of which can irritate the lips by extracting moisture and causing evaporation. Some children have the habit of sucking and biting the lower lip, whereby a sharply bordered perioral erythema may occur.
Cheilitis simplex.
Differential diagnosis includes contact cheilitis, atopic cheilitis, actinic cheilitis, etc. (2, 4). Therapy mostly involves advice on dealing with environmental conditions and the application of lip balms, petroleum jelly, emollients and sometimes topical corticosteroids, mostly low potency ointments.
Angular cheilitis (also termed perleche, cheilosis, or angular stomatitis or angulus infectiosus) typically manifests at the corners of the mouth/lips. The disease is most common in patients with deep wrinkles in lip angles and those who are prone to licking lip corners (8). Generally, the disease starts during vitamin and mineral deficiencies (B vitamins, iron, zinc, etc.), or is caused by other conditions and diseases (e.g., poorly fitting dentures and drooling, celiac disease) (4, 6, 9). An important factor is also saliva production, i.e. increased secretion and drooling, which contributes to the disease. Conversely, during decreased saliva secretion (hyposalivation), dryness promotes cracking and desquamation, as well as the invasion of Candida albicans with the emergence of angular cheilitis inflammation.
Angular cheilitis occurs more commonly in diabetics, in patients with some psychiatric disorders (e.g., lip trauma in bulimics or in anorexia nervosa), during certain drug therapy (e.g., isotretinoin), and somewhat less frequently in primary hypervitaminosis A. It is more common during winter when additional lip licking worsens the condition, and in elderly persons (2, 5). It can occur in patients with inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis (10).
This subtype sometimes develops as part of a group of symptoms, which can include atrophic glossitis, esophageal webs or strictures, and microcytic hypochromic anemia (Plummer-Vinson syndrome) (11). Concurrence of bacterial or candidal infection (primary or secondary) is common (2). Children, especially those with atopic dermatitis, are most commonly affected by secondary bacterial infections (staphylococcal and beta-hemolytic streptococcal) on damaged lip corners. Angular cheilitis with secondary infections often occurs also in patients with macroglossia (congenital hypothyroidism and Down syndrome).
Differential diagnosis for this type of cheilitis includes recurrent herpes labialis (if lesions are unilateral) and secondary syphilis (fissured papules at the corners of the lips similar to cheilitis) (2, 9). Therapy includes elimination of predisposing factors and often topical antimycotics, antiseptics, antibiotics, and sometimes corticosteroids.
Contact/eczematous cheilitis is an inflammatory lip reaction caused by the irritating or allergic effects of various substances found in many products such as lipsticks, oral hygiene products (toothpastes), food (e.g., eggs and crustaceans), ointment bases, fragrances, preservatives, antioxidants, dyes, dental materials, musical or occupational instruments, objects put in the mouth daily (e.g., nails, needles, pens), etc. (7, 12). It manifests as dryness, scaling, erythema or fissuring, more commonly on the skin than on mucosa (Fig. 2) (2, 13, 14). This type of cheilitis usually presents in patients with atopic dermatitis (15). Some authors use the term cheilitis venenata, which specifically indicates contact reaction, most commonly of an allergic type.
Contact/eczematous cheilitis.
There is a broad spectrum of products with common irritants and allergens associated with this subtype. Contact reactions to lipsticks, rubber, leather objects, nail polish substances (e.g., formaldehyde), metals (nickel, cobalt, gold) and topical antibiotics have been shown to be some of the more frequent etiologic factors (7, 12). Reactions to compounds in topical medications and medical products, such as topical antibiotics, virostatic agents, disinfectants, local anesthetics, and sunscreens are also possible. Factitial cheilitis stands out as a distinct subtype of contact cheilitis, usually triggered by a stressful event (possible self-damaging behavior).
Scientific investigation of factitious cheilitis psychosomatic ethiology
Scientific investigation of factitious cheilitis psychosomatic ethiology
J Med Case Reports. 2008; 2: 29.
Published online 2008 Jan 29. doi: 10.1186/1752-1947-2-29
PMCID: PMC2266766
PMID: 18226274
Factitious cheilitis: a case report
Erdinc Aydin,corresponding author1 Ozgur Gokoglu,1 Gamze Ozcurumez,2 and Hakan Aydin3
Author information Article notes Copyright and License information Disclaimer
Go to:
Abstract
Introduction
Factitious cheilitis is a chronic condition characterized by crusting and ulceration that is probably secondary to chewing and sucking of the lips. Atopy, actinic damage, exfoliative cheilitis, cheilitis granulomatosa or glandularis, contact dermatitis, photosensitivity reactions and neoplasia should be considered in the differential diagnosis of crusted and ulcerated lesions of the lip.
Case presentation
We present a 56 year-old female with an ulcerated and crusted lesion on her lower lip. The biopsy showed granulation tissue and associated inflammation but no malignancy. Based on the tissue examination and through clinical evaluation the diagnosis of factitious cheilitis was rendered.
Conclusion
Thorough clinical history, utilization of basic laboratory tests and histopathologic evaluation are required to exclude other diseases and a thoruough psychiatric evaluation and treatment is vital for successful management of these patients.
Go to:
Introduction
Self induced disorders may have variable presentations and they may roughly be classified into two groups. The ones with the characteristics of both impulsivity and compulsivity, patients usually acknowledge the self-inflicted nature of the lesions, typical examples of which are pychogenic excoriation (pathological or compulsive skin picking) and trichotillomania (chronic hair pulling) [1]. The other group constitutes abnormal illness behaviors in which patients have concious symptom formation but with motivations that arise from unconcious conflicts ie. Factitious disorders. An important distinction between these two groups of self-inflicted disorders is in the first group patients report their concern and they very much wish to put an end to their behavior while in the second group patients simulate, induce, or aggravate illness, often inflicting painful, deforming, or even-life-threatening injury on themselves primarily to gain the emotional care and attention that comes with playing the role of the sick. Factitious cheilitis, also known as factitious lip crusting, localized crusting or artifactual and exfoliative cheilitis, is a chronic condition characterized by crusting and ulceration [2-4]. It is attributed to self induced trauma such as repetitive bitting, picking or licking of the lips [5]. Preponderance in young women have been reported but it could be seen in any age group and race [2,3,6]. The lesions may be bizarre and hemorrhagic giving clinically a malignant impression [6].
Go to:
Case presentation
56 year-old female presented to the otolaryngology department with the chief complaint of a lesion on her lower lip. The lesion was first noticed by the patient 4 years ago and slowly increased in size. Her past medical history was unremarkable. She was not a smoker and there was no weight loss. Physical examination showed a painless, firm, indurated, crusted area of 4 cm with central ulceration giving the lip a bitten off appearance (Figure (Figure1).1). Otherwise skin and oral mucosa were normal. There were no palpable or ultrasonographically detected lymph nodes. CBC, sedimentation rate, and routine serum chemistries were all within normal limits.
An external file that holds a picture, illustration, etc.
Object name is 1752-1947-2-29-1.jpg
Figure 1
Photograph of an indurated, crusted lesion with central ulceration giving the lip a bitten off appearance.
An incisional biopsy that included the normal mucosa and skin was obtained. Histopathological examination showed a non-specific ulcer with inflammation and granulation tissue. There was no cellular atypia in favor of malignancy. Upon detailed history the patient declared her habit of bitting and sucking of the lip that was exacerbated during periods of stress. The patient did not seem gravely concerned about her lesion, nor did she admit to her habit of lip chewing but nevertheless was willing to undergo incisional biopsy. A diagnosis of factitious cheilitis was made and discussed with the patient with a following psychiatry consult. In the meantime, treatment was initiated with petrolatum ointment, chlorhexidine gluconate mouthwash and topical steroids. She refused psychiatric treatment of any kind including the prescribed selective-serotonin reuptake inhibitor (Fluoxetine 20 mg/day). After a year from her first presentation to otolaryngology department her lesion neither healed nor got better.
Go to:
Discussion
The exact pathogenesis of factitious chelitis is obscure. Although factitious illness behavior is, by definition, consciously produced, the underlying motivations for the behaviors are largely considered to be unconscious. Despite potentially high stakes, relatively little empirical knowledge is available about the etiology, epidemiology, course and prognosis, and effective treatment of factitious disorders. Methodological problems are inherent in the study of these deceptive patients, as they are difficult to identify, and, when found out, they often flee to avoid charges of fraud [7]. The pyschogenic cause was proposed by Brocq in 1921, who suggested a nervous instability [2]. Schaffer et al. draw attention to borderline personality disorder in factitial dermotosis [3,8]. Coping deficits are widely noted for the etiology of factitious illness behavior. Patients often have immature coping skills, not falling into any current category of personality disorder. This is consistent with observations that many factitious disorder patients come from large families or have been neglected as children, therefore lacking the nurturing conducive to the development of mature coping. On the other hand poor coping may be part of a personality disorder, such as borderline personality or dependent and narcissistic personality traits [5,9].
Our patient strongly opposed psychiatric intervention of any kind which is usually a typical feature of factitious disorder patients. Since she refused further psychiatric evaluation we do not have enough data to have an insight about her past, her personality, her relationship patterns and her coping skills. It is important to note that the psychiatric consultant diagnosed her depression and it is a known fact that factitious illness behavior often occurs in the setting of a loss and emotional turmoil [10]. So the inciting events for factitious illness behavior in our case might be her husband’s death which is followed by the departure of her daughters from home. The last blow probably came with the stress of being the sole caregiver for her demented father with whom she lives with for the last five years. Factitious illness behavior can be a maladaptive way of coping with stress and does not necessarily imply an ongoing factitious disorder. This might just be the case for our patient when we consider her living conditions for the last five years together with her untreated depression. Securing the attention of clinicians, family, and friends may be a way of obtaining emotional solace without directly confronting her losses. She might have anger rooted from the obligation of taking care of her demented father on her own and such feelings induce guilt that is extremely hard to cope with most of the time. Especially knowing that one of her daughters is a physician makes these speculations more salient. Her emotional needs and need for recognition and support might only be fullfilled by her factitious cheilitis. Laboratory studies did not support an organic etiology and biopsy findings were not contributory beyond that confirmation of physical findings. Although no laboratory or pathology tests are diagnostic of factitious disorders, they may be useful in demonstrating deception and helping to confirm diagnosis which is usually the case [7]. Some data suggests an associated thyroid abnormality [11,12]. In our patient thyroid function tests were normal.
Atopy, actinic damage, cheilitis, contact dermatititis, photosensitivity reactions and neoplasia should be considered in the differential diagnosis of crusted and ulcerated lesions of the lip [11,13]. Also hypervitaminosis A, lupus erythematosus and licenoid dermatosis have to be ruled out [2,11,13]. Cultures and histopathologic examination are prudent to rule out malignancy and specific infectious etiology. In this case, the patient’s history, the negative biopsy findings and a thorough clinical evaluation-including the psychiatry consultation – excluded organic causes.
Psychopharmacological and psychotherapeutic treatments should be used first line according to the diagnosis, depending on the presence of a comorbid DSM-IV (Diagnostic and Statistical Manual of Mental Disorders) Axis I disorder (eg. depression) or a comorbid Axis II disorder (eg. borderline personality). Other than targeting comorbid psychiatric disorders, there is no standard pharmacological treatment for factitious disorder. And one must have to keep in mind that an underlying mood or anxiety disorder that is treatable bodes for a better prognosis, whereas an underlying personality disorder bodes for a poorer prognosis [7]. Topical application of %20 urea, corticosteroids, antibiotics, antifungal agents, petrolatum gels and sunscreens are dermatological treatment agents [2]. However, the response rate is not promising as in our case. Exacerbations are associated with stress and have been shown to regress with psychotherapy and antianxiolytic-antidepressant treatment [2,5,14].
Go to:
Conclusion
Factitious cheilitis should be distinguished from infectious cheilitis, contact dermatitis, actinic cheilitis, photosensitivity dermatoses, exfoliative cheilitis, cheilitis glandularis and neoplasia that may look similar on physical exam. Bizarre hemorragic or keratotic crusts should alert the clinician to a possible factitious origin. We noticed that there is an interchangeable usage of exfoliative cheilitis and factitious cheilitis in the literature [5,6,11], however the differentiation of these two has clinical significance.
We suggest exfoliative cheilitis is a disorder where patients impulsively/compulsively induce the lesions without any primary goal of attaining the emotional care and attention that comes with the sick role, whereas in factitious disorder the lesions are intentionally produced with the primary goal of the sick role and these patients deny the self inflicted nature of their lesions at all cost. We think that making this differentiation is important in terms of further psychiatric intervention and treatment modalities. As self-inflicted disorders of compulsivity-impulsivity spectrum mostly benefit from selective-serotonin reuptake inhibitors with or without combined low doses of atypical antipsychotics, factitious disorders have to be handled with much more versatile modalities depending on the underlying pathologies. Thorough clinical history, utilization of basic laboratory tests and histopathologic evaluation are required to exclude other diseases and a thoruough psychiatric evaluation and treatment is vital for successful management of these patients.